Why complete QI?
Measure quality improvements in patient health outcomes
By participating in QI in your practice, you can identify opportunities to make changes that will improve patient health outcomes. All members of the practice team need to have the opportunity to contribute to your practice’s QI activities. When completing QI you identify areas of improvement related to patient data, patient feedback, systems improvement, increased knowledge, or evidence. GPs and practice teams should reflect on their own performance and engage in QI initiatives to improve the individual’s patient health outcome.
Meet RACGP accreditation requirements
The Royal Australian College of General Practitioners (RACGP) has developed the Standards for general practices (5th edition) (the Standards) with the purpose of protecting patients from harm by improving the quality and safety of health services. The Standards also support general practices in identifying and addressing any gaps in systems and processes. There are several standards relating to QI including:
QI Standard 1 – Quality Improvement - Our practice undertakes quality improvement activities to support the quality of care provided to our patients.
QI Standard 2 – Clinical indicators – Our practice records and uses patient data to support quality improvement activities
QI Standard 3 – Clinical risk management – Our practice has clinical risk management systems to improve the safety and quality of our patient care.
More information about the Standards is available from RACGP.
Meet Practice Incentive Program (PIP) requirements
Practice Incentive Program for Quality Improvement
The Federal Government’s Practice Incentive Program (PIP) encourages general practices to provide quality care, build and enhance their clinical capacity and improve accessibility and health outcomes for patients through a range of incentives.
The PIP Quality Improvement (PIP QI) incentive is a quarterly payment given to practices to undertake and provide evidence of continuous QI by:
providing the PIP Eligible Data Set (de-identified data) to the Primary Health Network (PHN)
participate in continuous quality improvement activities in partnership with their local PHN.
Practices may focus their QI activities on specified improvement measures. There are no set targets for the improvement measures.
About the PIP QI measures
The 10 improvement measures for the PIP QI have been identified to support understanding of chronic disease management in areas of high need. They facilitate a common data baseline and data analysis to observe improvements within general practice.
There are no prescribed targets associated with any of the improvement measures. Practices may choose to focus their QI activities on the specified measures or alternatively, focus on any other areas informed by their clinical information system data.
The 10 improvement measures:
1. proportion of patients with diabetes with a current HbA1c result
2. proportion of patients with a smoking status
3. proportion of patients with a weight classification
4. proportion of patients aged 65 and over who were immunised against influenza
5. proportion of patients with diabetes who were immunised against influenza
6. proportion of patients with COPD who were immunised against influenza
7. proportion of patients with an alcohol consumption status
8. proportion of patients with the necessary risk factors assessed to enable CVD assessment
9. proportion of female patients with an up-to-date cervical screening
10. proportion of patients with diabetes with a blood pressure result.
These measures may be altered to reflect emerging high-need areas regionally and nationally. The Quality Improvement Toolkit: PIP QI Ten Measures guides you through how to implement these 10 improvement measures.
Assist your GPs to meet their CPD hours
RACGP QI & CPD points for completing in quality improvement
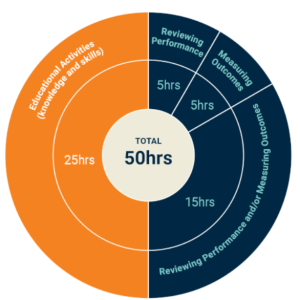
GPs are required to complete Reviewing Performance or Measuring Outcomes hours as part of the current triennium. More information is available from RACGP.
The Quality Improvement team are available to assist GPs to meet these criteria. The team can assist with:
identifying an area for improvement in the practice (patient related, systems improvement, data cleansing etc.)
planning how GPs will work towards their improvement (who will be involved, what will be done, how will any improvements be measured)
working through the planned steps
reviewing results.
Note: GPs can report the number of hours working on QI by contacting the CPD home.
The team have created 3 activities for measuring outcomes that have been pre-approved by the RACGP. Use these resources as a step-by-step guide.
Assessing and reviewing patients with a moderate complexity score
Reviewing patients who may need a clinical review for undiagnosed diabetes
Contact us for more support
Our Quality Improvement Team works with general practices to provide practical advice and resources to help plan, implement, and review your QI activities. To request further practice support, please contact the Quality Improvement team on Phone: 3864 7540 or email: support@bsphn.org.au.
Our team is dedicated to providing the best possible support for your practice.





